Managing diverticulitis often requires careful dietary adjustments, and understanding a proper liquid diet can be crucial for recovery. When diverticulitis flares up, healthcare providers frequently recommend liquid diets to allow the digestive system to rest and heal. This comprehensive guide will help you understand the different types of liquid diets, appropriate foods and beverages, and how to safely navigate this important phase of treatment under medical supervision.
Understanding Diverticulitis and Why Liquid Diets Help
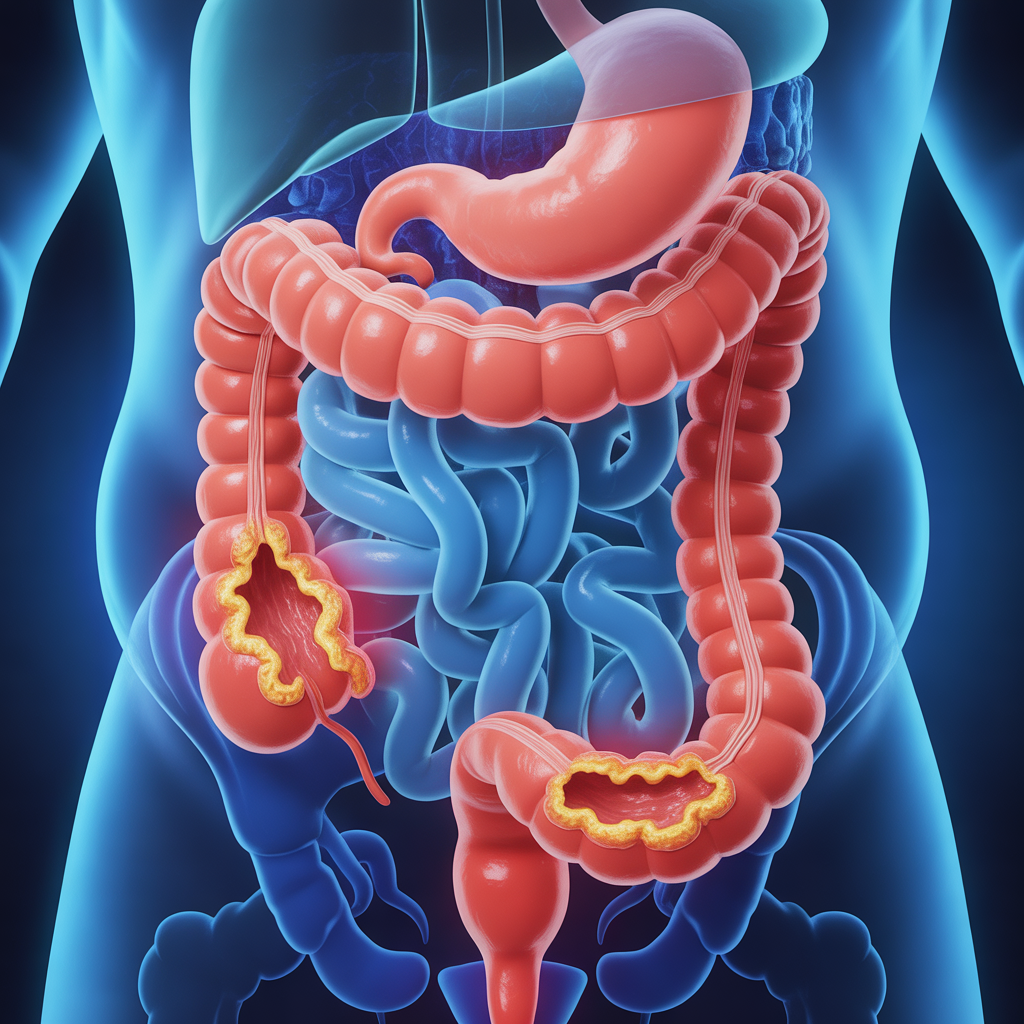
Diverticulitis occurs when small pouches called diverticula in the colon wall become inflamed or infected. Unlike diverticulosis, which is the presence of these pouches without symptoms, diverticulitis involves active inflammation that can cause significant discomfort and complications if not properly managed.
Common symptoms of diverticulitis include sharp abdominal pain (typically on the lower left side), fever, nausea, vomiting, and changes in bowel movements. The severity can range from mild discomfort to severe inflammation requiring immediate medical attention.

Liquid diets serve a specific therapeutic purpose during diverticulitis flare-ups. By consuming only liquids, the digestive system experiences reduced workload, allowing inflamed tissue to heal more effectively. This bowel rest approach helps minimize mechanical irritation to the affected areas while ensuring the body receives necessary hydration and some nutritional support.
Healthcare providers typically prescribe liquid diets during acute episodes to prevent complications such as perforation, abscess formation, or bowel obstruction. The duration and type of liquid diet depend on the severity of symptoms and individual patient factors, making medical supervision essential throughout the process.
It’s important to understand that liquid diets for diverticulitis are temporary therapeutic interventions, not long-term eating plans. Most patients can gradually return to solid foods as inflammation subsides and symptoms improve under their healthcare provider’s guidance.
Types of Liquid Diets for Diverticulitis Management
Medical professionals typically recommend two main types of liquid diets for diverticulitis, each serving different purposes depending on the severity of symptoms and stage of recovery.
Clear Liquid Diet
A clear liquid diet consists of transparent fluids that leave minimal residue in the digestive tract. This restrictive approach provides maximum bowel rest while maintaining hydration. Clear liquids are easily absorbed and require virtually no digestive work from the intestines.
Healthcare providers often recommend clear liquid diets during the most acute phases of diverticulitis when inflammation is severe. This diet typically lasts 1-3 days, though duration varies based on individual response and symptom improvement.
Clear liquid diets provide limited calories and virtually no protein, making them unsuitable for extended periods without medical supervision and possible nutritional supplementation.
Full Liquid Diet
Full liquid diets include all clear liquids plus opaque liquids that become liquid at room temperature. This approach provides more nutritional value while still maintaining digestive rest. Full liquid diets typically follow clear liquid diets as patients begin to improve.
The increased nutritional content of full liquid diets makes them more sustainable for longer periods, though they still require careful monitoring to ensure adequate nutrition. Healthcare providers often use this transitional approach before reintroducing soft solid foods.
Full liquid diets can typically be maintained for several days to weeks when medically necessary, with proper attention to nutritional balance and supplementation as needed.
Clear Liquid Diet Guidelines and Approved Foods
Understanding which liquids are appropriate for a clear liquid diet is crucial for effective symptom management. The goal is to consume only transparent fluids that provide hydration without leaving residue in the digestive tract.
Approved Clear Liquids
Water forms the foundation of any clear liquid diet and should be consumed regularly throughout the day to maintain proper hydration. Ice chips can provide variety while contributing to fluid intake, especially helpful when nausea makes drinking difficult.
Clear broths including chicken, beef, and vegetable varieties provide flavor and some electrolytes. Choose low-sodium options when possible and ensure broths are completely clear without visible particles or fat globules floating on the surface.
Plain gelatin without fruit pieces, nuts, or other additives offers carbohydrates and can help satisfy hunger temporarily. Choose light-colored varieties and avoid those with artificial colors or suspended particles.
Clear fruit juices such as apple, white cranberry, and white grape juice provide carbohydrates and some vitamins. Strain juices if necessary to remove any pulp, and dilute with water if they seem too concentrated or cause stomach upset.
Sports drinks and electrolyte solutions help maintain proper mineral balance, especially important during periods of limited food intake. Choose clear or light-colored varieties without artificial colors.
Plain tea and coffee (without cream or milk) can be consumed, though caffeine should be limited as it may cause stomach irritation in some individuals. Herbal teas like chamomile or peppermint may provide additional soothing benefits.
Clear popsicles and ice pops made from approved clear liquids can provide variety and help with hydration, particularly when appetite is poor. Avoid those with fruit pieces, artificial colors, or dairy ingredients.
Foods and Drinks to Avoid
Dairy products including milk, cream, and yogurt should be completely avoided during clear liquid diet phases as they leave residue and can be difficult to digest during inflammation.
Fruit juices with pulp, such as orange juice or tomato juice, contain fiber particles that defeat the purpose of bowel rest. All cloudy or thick juices should be avoided.
Alcohol consumption should be eliminated entirely, as it can worsen inflammation and interfere with healing. Alcoholic beverages also contribute to dehydration and may interact with any prescribed treatments.
Carbonated beverages can cause gas and bloating, potentially worsening abdominal discomfort. The bubbles may also contribute to intestinal distension, which should be avoided during acute phases.
Full Liquid Diet Guidelines and Nutritional Considerations
Full liquid diets expand food options while maintaining the liquid consistency that allows continued digestive rest. This approach provides better nutritional balance while still supporting the healing process.
Approved Full Liquids
All clear liquids approved for the previous phase remain appropriate for full liquid diets. Additionally, milk and dairy products can be reintroduced if well-tolerated, providing important protein and calcium.
Smooth yogurt without fruit pieces or nuts can provide probiotics that may support digestive health, along with protein and calcium. Choose plain varieties or those with minimal added sugars.
Plain ice cream and sherbet can provide calories and enjoyment, though they should be consumed in moderation due to high sugar content. Avoid varieties with nuts, fruit pieces, or other solid additions.
Protein shakes and nutritional supplement drinks become crucial components of full liquid diets, helping to meet protein requirements and providing essential vitamins and minerals. Choose products specifically designed for nutritional completeness.
Pureed soups that have been strained to remove any solid particles can provide variety and nutrition. Cream-based soups can offer protein and calories, while vegetable-based options provide different nutrients and flavors.
Preparation Methods and Consistency Requirements
Proper preparation ensures foods meet the liquid consistency requirements while maximizing nutritional value. Blending techniques should create completely smooth textures without any lumps or particles.
When preparing soups, use a high-powered blender followed by straining through fine mesh to ensure no solid particles remain. Temperature should be comfortable for consumption, neither too hot nor too cold.
Smoothies should be blended thoroughly and may need straining if ingredients create texture issues. Focus on ingredients that blend completely smooth, such as bananas, protein powders, and liquid bases.
Sample Meal Plans and Practical Implementation
Having structured meal plans helps ensure adequate nutrition while maintaining dietary compliance. These examples provide guidance while allowing flexibility based on individual preferences and tolerances.
Clear Liquid Diet Sample Day
Morning meals might include clear chicken broth warmed to a comfortable temperature, providing sodium and some protein derivatives. Follow with apple juice for carbohydrates and vitamin C, and plain tea for additional fluids and warmth.
Midday options could feature vegetable broth for different flavors and nutrients, plain gelatin for carbohydrates, and a sports drink to maintain electrolyte balance. Space consumption throughout the morning to avoid overwhelming the stomach.

Evening consumption might include beef broth for variety in flavor and nutrients, white cranberry juice for different vitamins and taste, and a clear popsicle for satisfaction and additional hydration before sleep.
Throughout the day, maintain consistent fluid intake with water and ice chips, aiming for adequate hydration while monitoring tolerance and symptoms.
Full Liquid Diet Sample Day
Breakfast options expand to include a protein smoothie made with milk, protein powder, and banana, providing substantial nutrition to start the day. Add a glass of milk for additional protein and calcium.
Lunch might feature a strained cream soup for variety and nutrition, followed by a nutritional supplement drink to ensure adequate vitamin and mineral intake. These provide more substantial nutrition than clear liquids alone.
Dinner could include a different flavored pureed and strained soup, plain yogurt thinned to liquid consistency, and milk-based beverages for additional calories and protein before nighttime rest.
Nutritional Management and Preventing Deficiencies
Liquid diets, while medically necessary, present nutritional challenges that require careful attention to prevent deficiencies and maintain overall health during recovery.
Key Nutrients to Monitor
Protein intake becomes a primary concern during liquid diet phases, as many liquid options provide limited protein content. Adequate protein is essential for tissue healing and immune function during recovery from diverticulitis.
Vitamins and minerals may become deficient during extended liquid diet periods. B vitamins, vitamin D, iron, and calcium are particularly important to monitor, especially in longer-duration liquid diets.
Fiber intake drops dramatically during liquid diets, which is intentional for bowel rest but requires careful attention during the transition back to solid foods to prevent digestive disruption.
Hydration Strategies
Daily fluid requirements increase in importance during liquid diets since all nutrition comes from fluid sources. Aim for adequate hydration while balancing with symptom tolerance and medical recommendations.
Electrolyte balance requires attention, particularly sodium, potassium, and magnesium levels. Sports drinks and broths can help maintain proper mineral balance, but medical monitoring may be necessary.
Signs of dehydration include dark urine, dizziness, fatigue, and dry mouth. These symptoms require immediate attention and possible medical consultation to adjust fluid intake strategies.
Transitioning Back to Solid Foods Safely
The transition from liquid diets back to solid foods requires careful planning and gradual progression to avoid symptom recurrence and support continued healing.
Gradual Progression Steps
Low-fiber soft foods typically represent the first step away from liquid diets. These might include well-cooked white rice, plain pasta, white bread, and smooth nut butters, all of which provide more substantial nutrition while remaining easy to digest.
Slowly increasing fiber content follows successful tolerance of low-fiber options. Gradually introduce small amounts of soluble fiber sources like oatmeal, bananas, and well-cooked vegetables without skins.
Monitoring tolerance becomes crucial during each transition phase. Symptoms such as increased abdominal pain, changes in bowel movements, or digestive discomfort may indicate the need to slow the progression or return to previous dietary phases.
Safe Food Reintroduction
Recommended first solid foods include refined grains, lean proteins that are well-cooked and tender, and fruits without skins or seeds. These provide nutrition while minimizing digestive challenge.
Foods to continue avoiding temporarily include high-fiber items like nuts, seeds, popcorn, and raw vegetables. These foods may be reintroduced later but could potentially irritate healing tissue if introduced too early.
Portion size guidelines suggest starting with small amounts and eating slowly to assess tolerance before increasing quantity. This approach helps identify any foods that may cause symptoms while supporting continued recovery.
Managing Symptoms and When to Seek Medical Care
Understanding common side effects of liquid diets and recognizing when to contact healthcare providers is essential for safe management of diverticulitis recovery.
Common Side Effects of Liquid Diets
Fatigue and weakness commonly occur due to reduced caloric intake and limited protein consumption. These symptoms typically improve as nutrition is gradually restored, but they require monitoring to ensure they don’t become severe.
Hunger and cravings are normal responses to liquid diets, especially as symptoms improve and appetite returns. Psychological challenges around food restriction are common and usually temporary.
Mood changes including irritability, difficulty concentrating, and mild depression can occur with dietary restrictions. These typically resolve as normal eating patterns are restored, but support may be helpful.
Digestive changes such as decreased bowel movements are expected with liquid diets. However, significant changes or concerning symptoms should be discussed with healthcare providers.
When to Contact Healthcare Providers
Worsening symptoms including increased abdominal pain, fever, or changes in bowel movements require immediate medical attention, as they may indicate complications or inadequate treatment response.
Signs of complications such as severe abdominal pain, persistent vomiting, signs of dehydration, or inability to tolerate liquids need prompt medical evaluation and possible treatment modification.
Nutritional concerns including significant weakness, dizziness, or signs of deficiency should be addressed with healthcare providers who may recommend modifications or supplementation.
Frequently Asked Questions About Liquid Diets for Diverticulitis
Duration and Timeline Questions
The duration of liquid diets varies significantly based on individual symptoms, severity of inflammation, and response to treatment. Most clear liquid diets last 1-3 days, while full liquid diets may continue for several days to weeks under medical supervision.
Extending liquid diets beyond recommended timeframes requires medical consultation, as prolonged restriction can lead to nutritional deficiencies and other complications that may outweigh benefits.
Personal judgment about diet duration should always defer to medical professional guidance, as healthcare providers can assess symptom improvement and determine appropriate timing for dietary advancement.
Food and Drink Specifics
Protein powders are generally appropriate for full liquid diets when mixed to liquid consistency. Choose unflavored or mild varieties and ensure they dissolve completely without leaving particles.
Flavored waters without artificial colors or suspended particles are typically acceptable for clear liquid diets. Check ingredient lists to ensure compliance with clear liquid requirements.
Herbal teas can provide variety and potential therapeutic benefits, though individual tolerance may vary. Chamomile and peppermint teas are often well-tolerated and may provide additional digestive comfort.
Practical Concerns
Work capacity during liquid diets may be reduced due to lower energy levels and potential side effects. Discuss work modifications with employers if necessary and plan for potential fatigue or concentration difficulties.
Social situations can be challenging during liquid diet periods. Planning ahead, bringing appropriate beverages, and communicating dietary needs to others can help maintain social connections while adhering to medical requirements.
Liquid intolerance may occur with certain items due to individual sensitivities or inflammation severity. Alternative options within the same diet category can usually be found with medical guidance.
Conclusion and Key Takeaways
Liquid diets represent an important therapeutic tool in managing diverticulitis, providing necessary bowel rest while supporting the healing process. Understanding the differences between clear and full liquid diets, appropriate food choices, and proper implementation can significantly impact recovery outcomes.
The temporary nature of these dietary restrictions is important to remember, as they serve specific medical purposes during acute phases of illness. With proper medical supervision and careful attention to nutritional needs, most individuals can successfully navigate liquid diet periods and return to normal eating patterns.
Individual variation in response to liquid diets means that what works for one person may not be appropriate for another. Medical supervision ensures that dietary approaches are tailored to specific needs and circumstances, maximizing benefits while minimizing risks.
Professional guidance remains essential throughout the entire process, from initial diet implementation through gradual food reintroduction. Healthcare providers can monitor progress, adjust recommendations, and provide support during challenging aspects of dietary restriction.
Recovery from diverticulitis is possible with appropriate care, and liquid diets represent just one phase of comprehensive treatment. With patience, proper medical care, and adherence to dietary recommendations, most individuals can expect to return to normal eating and activities while learning valuable information about long-term digestive health management.

